About Choroidal Melanoma
What is Choroidal Melanoma?
Choroidal melanoma is a primary cancer of the eye. It arises from the pigmented cells of the choroid of the eye and is not a tumor that started somewhere else and spread to the eye. Malignant means that the tumor is a cancer which may metastasize, that is, spread to other parts of the body. Although some choroidal melanomas are more life-threatening than others, almost all should be treated as if they were malignant.
How is the diagnosis of choroidal melanoma made?
 Choroidal melanoma is diagnosed during an examination of the eye by an ophthalmologist. Your eye doctors are able to recognize a choroidal melanoma by the degree of pigmentation of the tumor, by its shape and location, and by other features observed in an eye examination. Unlike tumors in other parts of the body, choroidal melanoma is directly visible through the "window" provided by the pupil. Most of the time, the ophthalmologist can be nearly certain of the diagnosis from clinical appearance, photographs, and ultrasound pictures. Therefore, biopsy, which is often indicated to diagnose tumors in other parts of the body, is avoided.
Choroidal melanoma is diagnosed during an examination of the eye by an ophthalmologist. Your eye doctors are able to recognize a choroidal melanoma by the degree of pigmentation of the tumor, by its shape and location, and by other features observed in an eye examination. Unlike tumors in other parts of the body, choroidal melanoma is directly visible through the "window" provided by the pupil. Most of the time, the ophthalmologist can be nearly certain of the diagnosis from clinical appearance, photographs, and ultrasound pictures. Therefore, biopsy, which is often indicated to diagnose tumors in other parts of the body, is avoided.
Are there any tests which help in the diagnosis of choroidal melanoma?


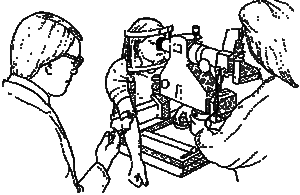
Some specialized tests which use sound waves (echography or ultrasound) and fluorescent dye (fluorescein angiography) may help your doctor to make the diagnosis of choroidal melanoma more certain. In the echography test, soundwaves are directed towards the tumor by a small probe placed on the eye.
The pattern made by reflection of the sound waves helps your doctor to diagnose the tumor.
 A test called fluorescein angiography also may be useful. In this test, a fluorescent dye is injected into a vein in the arm. As the dye passes through the blood vessels in the back of the eye, a rapid sequence of photographs is taken through your pupil. The appearance of the eye on these photographs may help your doctor to diagnose choroidal melanoma. Using the information provided by these tests, your doctor has been able to determine that your tumor is a "medium"-sized choroidal melanoma. Although it is classified as "medium," the melanoma is only about the size of a pea.
A test called fluorescein angiography also may be useful. In this test, a fluorescent dye is injected into a vein in the arm. As the dye passes through the blood vessels in the back of the eye, a rapid sequence of photographs is taken through your pupil. The appearance of the eye on these photographs may help your doctor to diagnose choroidal melanoma. Using the information provided by these tests, your doctor has been able to determine that your tumor is a "medium"-sized choroidal melanoma. Although it is classified as "medium," the melanoma is only about the size of a pea.
What happens when there is a choroidal melanoma in the eye?
Some choroidal melanomas appear to remain dormant and do not grow. Most enlarge slowly over time and lead to loss of vision. These tumors can spread to other parts of the body and lead eventually to death.
Why is treatment recommended?
Treatment of choroidal melanoma is recommended when your doctors judge that, on the basis of your medical history and the findings from the eye examination, your tumor is likely to enlarge and possibly spread to other parts of your body if left untreated.
What treatments are given for medium choroidal melanoma?
For 100 years or longer, the usual treatment for choroidal melanoma has been removal of the eye, or enucleation. If the tumor has not spread to other parts of the body, then removal of the eye rids the patient of the tumor.Since World War II, radiation treatment has been used for choroidal melanoma. During the past 20 years, this method of treatment has been refined. Radiation, at the appropriate dose rates and in the proper physical forms, is intended to eliminate growing tumor cells without causing damage to normal tissue sufficient to require removal of the eye. As the cells die, the tumor shrinks, but it usually does not disappear entirely. The most promising widely available method for irradiating medium choroidal melanoma involves constructing a small plaque with radioactive pellets glued to one side. Doctors who take care of patients who have choroidal melanoma are enthusiastic about the possibilities for this treatment, but satisfactory information about long-term results is not available. Your doctors recognize that they have a responsibility to current and future patients with choroidal melanoma to test radiation in a clinical trial.
High energy particles (helium ion or proton beam radiation) from a cyclotron also can be used to irradiate tumors. Surgery is performed first to sew small metal clips to the sclera so that the particle beam can be aimed accurately. Treatment is given over several successive days. The equipment needed for these treatments is available only in a few centers in the world. Good results have been reported in some patients, but many patients treated in this way have been followed for only a few years. Therefore, the long-term results of these forms of radiation therapy compared with the more commonly used plaque are unknown.
Over the years, other treatments have been used for a small number of patients. Photocoagulation using white light or laser light has been used to burn small tumors, and cryo-therapy has been used to kill the tumors by freezing them. These techniques are believed to work only for very small tumors. Some doctors have combined laser or cryotherapy with radiation, but such treatments are experimental. A few patients have had eye wall resection or a related procedure to remove tumors from their eyes. These methods of treatment are considered experimental by most doctors and have been used only for a small number of tumors. No treatment is available that can guarantee to destroy the tumor, to preserve vision, or to assure a normal lifespan.
How is enucleation performed?
For enucleation surgery, the patient is admitted to the hospital and the eye is removed under either local or general anesthesia. The enucleated eye cannot be treated or repaired and replaced in the eye socket. Instead, it is replaced with a ball implant that may be made of plastic or other materials. The implant is sewn into position and the eye is allowed to heal. The patient usually leaves the hospital one or two days after surgery. In some cases, patients are permitted to go home the same day. Three to six weeks later, a specialist who makes artificial eyes (called an ocularist) fits the patient with a prosthesis. The prosthesis is a plastic shell painted to resemble the other eye and inserted between the eyelids. When the other eye moves, the ball implant moves also, causing the prosthesis to move with the normal eye. Movement is usually less than that of the normal eye; however, the doctor and close relatives are most often the only people to notice that the patient does not have two normal eyes. If you have questions about different types of implants, be sure to ask your doctor. The purpose of the implant is to replace the volume in the socket that had been taken up by the eye.
Eye movements after removal of the right eye
What are the consequences of enucleation?
Enucleation surgery removes the tumor from the body if no spread outside the eye has occurred. Unfortunately, loss of vision for the eye removed is permanent because an entire eye cannot be transplanted. There is a reduced visual field on that side of the body when looking straight ahead, and there is loss of depth perception (stereopsis) as well. You can imagine what enucleation would be like by closing or patching one eye. Many of the skills of depth perception may be relearned with time; thousands of people have lost one eye and continued to live normal, productive lives. The book A Singular View, The Art of Seeing With One Eye, by Frank B. Brady is an excellent reference.Although the cosmetic results after removal of the eye and fitting of an artificial eye are usually good, the eye often does not move as well as the natural eye. There also may be some differences in the position of the eyelids when compared to the natural eye and the position of the artificial eye may look slightly abnormal. Despite these potential problems, the cosmetic appearance after enucleation is usually quite good.
After enucleation there may be some temporary pain which can be relieved by medication. Possible surgical complications include hemorrhage, complications of anesthesia, and late infection requiring removal of the implant. These serious problems are rare. Several years ago a suggestion was made that enucleation surgery might promote spread of tumor cells into the bloodstream during the operation and thereby lead to a reduced lifespan for the patient. This theory has never been proven and is not generally accepted. It is important to know that enucleation surgery for melanoma, like all cancer surgery, is performed in a way to minimize the possibility of spreading the cancer during the operation. Radioactive plaque therapy and eye wall resection also involve significant surgical manipulation of the eye. Thus, the risk of spreading the tumor by surgical manipulation is probably the same with enucleation as with other forms of therapy requiring surgery.
How is radiation performed for medium choroidal melanoma?
 When using radiation to treat medium choroidal melanoma, the goal is to destroy the tumor and save the eye. If the eye is to be saved, it is important to give high doses of radiation to the tumor and very little to the rest of the eye. This goal often can be accomplished with a small radioactive plaque sewn or sutured to the outside of the eye over the base of the tumor. This type of radiation procedure is sometimes called brachytherapy. The plaque is constructed with radioactive iodine seeds or pellets (A) glued to one side (B) and a thin gold sheet (C) attached to the other. Since gold stops this particular type of radiation, it acts as a shield to protect the parts of the head around the eye from radiation damage, especially those tissues beyond the shield.
When using radiation to treat medium choroidal melanoma, the goal is to destroy the tumor and save the eye. If the eye is to be saved, it is important to give high doses of radiation to the tumor and very little to the rest of the eye. This goal often can be accomplished with a small radioactive plaque sewn or sutured to the outside of the eye over the base of the tumor. This type of radiation procedure is sometimes called brachytherapy. The plaque is constructed with radioactive iodine seeds or pellets (A) glued to one side (B) and a thin gold sheet (C) attached to the other. Since gold stops this particular type of radiation, it acts as a shield to protect the parts of the head around the eye from radiation damage, especially those tissues beyond the shield.
 For placement of a radioactive plaque, the patient usually is admitted to the hospital. Surgery under local or general anesthesia is required and usually takes one to two hours. An incision is made in the conjunctiva, a thin membrane which covers the outside of the eye, and the radioactive plaque is stitched to the outside of the eye over the tumor. The conjunctiva is then sewn back over the plaque. In many medical centers, the patient stays in the hospital until the plaque is removed. After approximately three to seven days, surgery is performed again to remove the plaque. (Careful calculations determine how long the plaque must remain in place to give the tumor the proper amount of radiation.) Surgery for removal of the plaque takes less than an hour, under either local or general anesthesia, and often the patient can go home later the same day.
For placement of a radioactive plaque, the patient usually is admitted to the hospital. Surgery under local or general anesthesia is required and usually takes one to two hours. An incision is made in the conjunctiva, a thin membrane which covers the outside of the eye, and the radioactive plaque is stitched to the outside of the eye over the tumor. The conjunctiva is then sewn back over the plaque. In many medical centers, the patient stays in the hospital until the plaque is removed. After approximately three to seven days, surgery is performed again to remove the plaque. (Careful calculations determine how long the plaque must remain in place to give the tumor the proper amount of radiation.) Surgery for removal of the plaque takes less than an hour, under either local or general anesthesia, and often the patient can go home later the same day.
What are the consequences of radiation treatment?
When radioactive plaque therapy is successful, the tumor stops growing and may shrink over the course of 6 to 12 months. The patient keeps his or her own eye and, in favorable circumstances, when the tumor responds well and is located away from the most important parts of the eye, the tumor is destroyed and the patient may be able to see with the eye.Radiation from a radioactive plaque does not always destroy or inactivate the tumor. The tumor may grow and the eye may have to be removed at a later time. Delaying removal of the eye may allow the tumor to spread elsewhere in the body.
Radioactive plaque therapy requires two operations. Risks during surgery are similar to those described earlier for enucleation surgery. Compared to enucleation, there are added costs for a second operation, for the radioactive plaque, and for a longer hospital stay. Radiation almost always damages some healthy parts of the eye. Radiation damage to the blood vessels of the retina (radiation retinopathy) or to the optic nerve often causes a gradual loss of vision. In some cases, hemorrhage (bleeding) into the inner part of the eye (vitreous cavity) may occur and cause loss of vision. Radiation damage to the lens may cause a cataract, which may require removal by surgery sometime later.
After radioactive plaque treatment, many patients note some dryness and irritation of the eye which usually can be relieved by use of eye drops called artificial tears. In some instances, eyelashes may be permanently lost. In rare instances the outside layer of the eye (sclera) may become very thin. Occasionally, there may be prolonged redness, irritation, or infection inside the eye. The patient may see double if the muscles are damaged during the operation to apply or remove the plaque.
Continue with About the COMS
Return to COMS Home Page
Copyright © 1997, 1999, 2000, The Collaborative Ocular Melanoma Study.
All rights reserved.